10 May Vitreous Hemorrhage and Diabetes
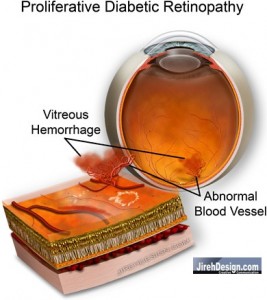
A vitreous hemorrhage can result in sudden, painless loss of vision. In patients with diabetes, the cause may be due to either a posterior vitreous detachment (PVD) or proliferative diabetic retinopathy (PDR). Remember, the proliferative phase of the diabetic retinopathy means that there are areas of neovascularization (abnormal blood vessel proliferation) on the surface of the retina.
In cases where a diabetic patient is diagnosed with a vitreous hemorrhage, my job is to ensure that the cause is not due to a retinal tear or a retinal detachment. This can be done by dilating the eye and examining.
You Can’t See Out and I Can’t See In
Sometimes there is so much blood I can not see much or any of the retina. In these cases, we perform an ultrasound of the eye to make sure the retina is attached.
Sometimes, an ultrasound can locate a retinal tear. If there is no retinal tear, or retinal detachment, then I am pretty sure that the vitreous hemorrhage is due to the proliferative diabetic retinopathy.
Fragile Vessels
Neovascular vessels are very fragile and may easily break open and bleed. This may occur with or without straining. The blood can fill the vitreous cavity causing sudden “loss” of sight. Vision is “lost” (not permanently) due to physical blockage of light.
Bleeding in the vitreous is benign. It causes no damage to the vision or to any part of the eye. On the other hand, as it physically blocks light, patients don’t see well.
Sometimes it is Best to do Nothing
Usually, when I am sure the bleeding is due to diabetic retinopathy, I recommend a period of doing nothing. We watch and wait. In doctor lingo, we are observing.
Patients Tire of Not Seeing
After a few weeks, or sometimes longer, we may decide to operate to remove the blood. Sometimes the blood absorbs on its own and sometimes it doesn’t. At some point, patients with non-absorbing blood in the eye become tired of the prolonged decreased vision. A vitrectomy is then scheduled to remove the blood.
What Does This Mean? The sudden loss of vision can be devastating for anyone. In cases when the loss of vision is due to a vitreous hemorrhage, we need to assess the threat of permanent vision loss due to other causes such as a retinal tear or retinal detachment.
If the eye is stable, that is, we can safely observe, it is sometimes tough to reassure patients that while they just “lost” their vision, the best idea is to do nothing! Their “lost” vision is temporary.
I often will have a patient return in a short week or two to reassess and help relieve anxiety.
Patients with proliferative diabetic retinopathy, if you remember, will require laser treatment (pan-retinal photocoagulation, aka PRP) to reverse the neovascularization.
While we are waiting for the hemorrhage to clear, at the same time we are mindful that laser treatment is ultimately needed. If the vitreous hemorrhage clears by itself, laser can be applied in the office. If we end up operating, the laser can be applied at the same time as the vitrectomy.

![Reblog this post [with Zemanta]](http://img.zemanta.com/reblog_e.png?x-id=40f2fa85-ffec-4079-a3e0-3ee0a403531b)
Althea Grange
Posted at 12:06h, 30 DecemberIf I have no vision in right eye and vitreous hemorrhage in left eye due to diabetic and a retinal tear and could not see how to drive nor read, would I be able to work?
Randall V. Wong, M.D.
Posted at 11:11h, 31 DecemberDear Althea,
I guess it really depends upon what type of work you do. Can you read this?
Make sure that someone, likely a retinal specialist, takes a look at you.
Best of luck.
Randy
ranjeet singh
Posted at 08:56h, 28 Maymy elder cousin sister (age 40 ), one day she was teaching her daughter then suddenly shr=e lost the view of her left eye tell me wat it could be doctor says it is vitreous hameerge its been more then 2 months she is not able to see tell me she has to operate or it will be ok automaticaly witouht operation ,
thanks
Randall V. Wong, M.D.
Posted at 11:08h, 29 MayDear Ranjeet,
A vitreous hemorrhage, by itself, does not cause a problem, but the cause of the vitreous hemorrhage can be problematic.
Is your cousin diabetic?
Randy
Aejaz ahamed
Posted at 08:45h, 08 JulyI am diabetics patient since 20 years and have undergone diabetics retinopathy surgery due to bleeding in eye doctor says i have to wait for 2 months for my vision .i am 40 years old weather i will get my vision or not please reply with your valuable advice thank you sir.
Randall V. Wong, M.D.
Posted at 09:48h, 11 JulyDear Aejaz,
I can better help you if I know how good or bad your vision was prior to surgery, and why did yo have surgery?
Often, my patients get some bleeding after surgery and it takes several weeks for the blood to absorb. I don’t know if this is the case with you and would encourage you to ask your surgeon.
Good luck. Write back and let us know how you are doing!
Randy
Aejaz ahamed
Posted at 11:21h, 12 JulyDear sir,
thanks for your reply,i have undergone before my operation laser treatment non proliferative diabetic ratinophathy 14 times..now after the bleeding in my right eye the doctor has done this operation .
diagnosis:-
summary :- ou-lasered -proliferative diabatic ratinophathy..
-od-cataract
premacular haemorrhage
-os -vitreomacular traction
Treatment done-
-od -parspalna -vitrectomy+membrane peeling ++ endolaser +intravitreal triam cinolone-asitonide+phacoemol sication +10 L -Done-under-LA -ON 22/6/2011
Previous to this operation i had blurred vision
the eye on which i had operation , i am unable to see anything from it,.
can you plz tell how many weeks it make taketo get the vision back
with regards,
Aejaz
gfry
Posted at 19:10h, 13 Decemberwhat about PDR with vitrous haemorrhage and glucoma developed in the affected eye
Randall V. Wong, M.D.
Posted at 15:07h, 21 DecemberDear gfry,
Yes, PDR can lead to neovascular glaucoma.
Randy
Kandice
Posted at 13:20h, 27 MayI’m 20 years old and got hit in the eye, which resulted in a small bruised and a small spot of blood inside the vitreous, in the right corner of my right eye. Within days it changed and over the last three months it has gotten lighter, but it still has not gone completely. I can see fine through my eye, as of now it’s only a nuisance. My question is how much longer can I expect for this to clear up?
Randall V. Wong, M.D.
Posted at 15:20h, 04 JuneDear Kandice,
If this is indeed located within the vitreous, it may linger for months…or longer.
r
Worried Diabetic
Posted at 20:41h, 22 AugustDrar Doctor
I have proliferative diabetic retinopathy, and just had a vitreous hemmorage (2 months ago). I also have a slight PVD. I have many “spider webs” in my vision, and some areas are very blurry. But I have a “clearer” area right in the centre (with a “ring” around it). Does that make sense? My vision seems to get better and worse over time. Sometimes I think it is really clearing up, and then the next day it’s more blurry. Can you help me understand why this is happening?
Most sincerely
Worried Diabetic
Randall V. Wong, M.D.
Posted at 08:00h, 28 AugustDear Worried Diabetic,
Most likely you have “clots” of blood in the vitreous and you get a heterogeneous (unequal) distribution of blood throughout the gel inside your eye. Therefore, you’ll notice some areas clearer than others.
I bet things have improved since 8/22?
r
Worried Diabetic
Posted at 12:44h, 28 AugustThanks You Doctor
It has improved (I think), but every slightly. It’s been very furstrating and I don’t know if it’s time to start thinking about a vitrectomy??? How I fear the surgery for the risk of going completely blind in that eye. I also see one “strand” that seem “rooted” and will not swoosh away….everything else seems “fluid in my eye”.
It’s even to the point where I’ve gained 8 pounds already, as I am petrified of swimming or exercising in fear I will cause another hemmhorage. Are these related?
Randall V. Wong, M.D.
Posted at 08:35h, 03 SeptemberDear Worried Diabetic,
Get back to exercising. Exercise and the blood are not related.
Vitrectomy is not a bad thing. It can:
1. Remove blood and allow treatment to proceed.
2. Give you piece of mind by “getting this over.”
3. Vitrectomy is as safe or safer than cataract surgery…to put things into perspective.
r
Worried Diabetic
Posted at 19:17h, 12 OctoberDear Doctor
Thank-you for your help during these difficult times. I must say your expert advice puts me at ease. So I went forward with the vitrectomy. I was nervous and very scared, but as you said, things went well and my vision has returned. I’m just in the phase of having the bubble reabsorb. Thank goodness we did the procedure, as I also had a retinal tear (that we were unaware of because we could not see into eye due to amount of blood). Do you know when is the highest chance for a rebleed to occur (I was told ~20% of people experience tihs). I’m just wondering when I’ll be “in the clear” from side-effects of the operation (including rebleed and infection). Most thankfully yours,
Worried Diabetic