19 Apr Gas Injection for Retinal Detachments
Injecting gas into the eye, called pneumatic retinopexy, is the fourth way to fix retinal detachments. Other methods include
- Scleral Buckle
- Vitrectomy Eye Surgery
- Combination of Scleral Buckle and Vitrectomy
Gas Injection
This procedure is performed in the office. Similar to other intraocular injections, except gas is introduced into the eye instead of anti-VEGF medications or steroids.
The gas is usually injected at 100% concentration and will expand a bit over the first day or so. This allows us to inject a small amount of gas that will enlarge and cover more retinal surface area.
Gases used are usually SF6 (sulfur hexafluoride), C2F6 (hexafluoroethane) and C3F8 (octafluoropropane). These are large molecules, are inert (don’t react with tissue) and can expand at given concentrations.
Their large size means that they will be slowly absorbed after injection, giving us plenty of time to use them as a tool. In comparison, air, if injected into the eye, does not expand and will be absorbed within 24 hours.
Advantages of Gas Injection
No “operation” is the biggest advantage. The procedure can be completed within hours of diagnosis. There are no issues with scheduling an operation at the hospital, pre-operative clearance and coordinating schedules.
Quick Healing – no actual cutting, so tissue healing is very quick.
No Change in Glasses – as the eye remains the same shape (in contrast to scleral buckle), there is no change in glasses prescription.
Disadvantages to Pneumatic Retinopexy
Lower Success Rate – not all retinal detachments can be treated with gas injection. The forces within the vitreous are NOT changed.
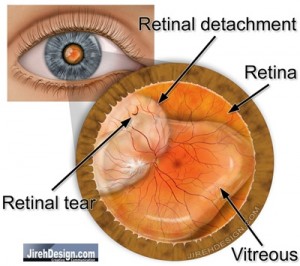
After gas is injected, the head must be positioned so that the gas abuts the retinal tear. For instance, if the tear is at the “12 o’clock” position of the eye, the head must be held upright, or erect. Similaryly, if the retinal tear is located at “9 o’clock” as you are looking at the patient, the head must be tilted over to the left to position the gas “bubble” appropriately.
For example, in the illustration above, the tear is located at 10 o’clock. The head should be tilted to the patient’s left, so the gas, as it rises in the eye, will abut the retinal tear.
Usually, only retinal detachments with tears from 8-4 o’clock can be treated with gas. It is not possible to treat tears occurring at 6 o’clock.
In both scleral buckle surgery and vitrectomy eye surgery, forces are reduced in the vitreous. This does not occur with pneumatic retinopexy (gas injection). Therefore, redetachment occurs more often. The success rate is lower, perhaps around 85% for this procedure. Scleral buckle and/or vitrectomy procedures are slightly more successful.
Whenever gas is used, there is a higher rate of cataract formation after the operation. As with any procedure, there is a chance of infection that can cause blindness.
How the Gas Bubble Works
Basically, the gas, when positioned properly, blocks the transmission of fluid through the retinal tear or retinal hole. The retina reattaches. By using either laser or freezing (cryotherapy), the tear is treated to induce scarring that will eventually “seal” the retina and prevent re-detachment. It does NOT “push” the retina back per se.
What Does This Mean? Depending upon the circumstances, there are a variety of ways to operate to fix a retinal detachment. Gas injection has many advantages, and is a successful way to proceed.
My personal feeling is that gas injection used to be a great time saver, however, the success rate is lower. As technology as advanced (e.g. 25 gauge vitrectomy), operating room procedures have become easier, and quicker, to perform. The advantages to pneumatic retinopexy, or gas injection, have become…well, er, “blurry.”

![Reblog this post [with Zemanta]](http://img.zemanta.com/reblog_e.png?x-id=143a3aa6-fa8c-48db-a6db-80c271585dab)
Khuzaima Saifudeen
Posted at 10:36h, 07 JulyI had a retinal tear on my right eye and went through a buckle surgary as explained to me by my doctor CHARITH FONSEKA (a popular local surgan in Sri Lanka) about two months ago. As the bubble became very small now I have what he calls a leak on the right side bottom and tomorrow morning he is going inject gas bubble again.
Is this correct ?
Randall V. Wong, M.D.
Posted at 14:49h, 12 JulyKhuzaima,
Could be that he is worried about the area detaching again. More gas could work.
Randy
Pingback:Gas Bubbles in Eye Surgery | Macular Holes
Posted at 19:00h, 22 April[…] a “gas bubble” into the eye is commonplace for certain types of retinal surgery. Not all retina surgery requires […]
peter riznyk
Posted at 15:35h, 14 NovemberI had a partial retinal tear that was repaired with one suture and laser and a gas bubble. About 60% of my gas bubble has resolved as I am now four weeks postop. I am planning a road trip and my surgeon told me to be careful with elevation. highest elevation is about 900 feet would that be enough to cause increased pressure to my gas bubble and cause problems with my vision?
Mike Rosco
Posted at 20:08h, 03 MarchHello Peter,
Apologies for the delay – we are just getting back into the groove here. You undoubtedly have already gone on your road trip; however, in the spirit of education, assuming you had your bubble placed at or around sea level, it will expand by 1.25 times at 5,000 feet, 1.5 times at 10,000 feet, and 2 times at 18,000 feet. A 900 foot increase in elevation would probably not pose any significant risks (especially at four weeks post op).
Hope you had a wonderful trip,
Mike Rosco, MD